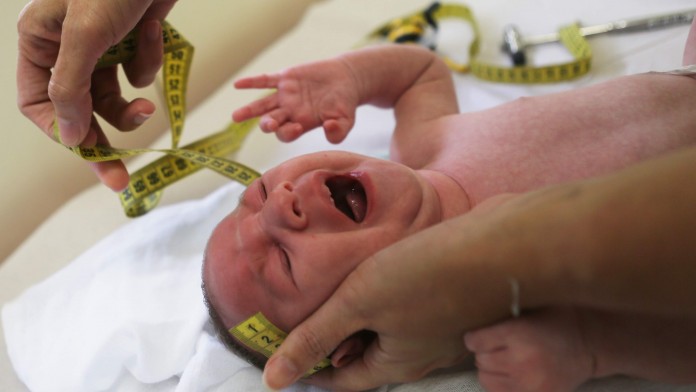
Federal health officials confirmed Wednesday that the Zika virus causes a rare birth defect and other severe fetal abnormalities, marking a turning point in an epidemic that has spread to nearly 40 countries and territories in the Americas and elsewhere.
Scientists at the Centers for Disease Control and Prevention conducted a careful review of existing research and agreed that the evidence was conclusive, Director Thomas Frieden said. It is the first time a mosquito-borne virus has been linked to congenital brain defects.
“It is now clear, and CDC has concluded, that the virus causes microcephaly,” Frieden said. CDC is launching more studies to determine whether children with that rare condition, which is characterized at birth by an abnormally small head, represent the “tip of the iceberg of what we could see in damaging effects on the brain and other developmental problems.”
The outcome validates the growing research of past months that strongly implicated Zika as the culprit behind a broad set of complications in pregnancy. The pathogen is also increasingly linked to neurological problems in adults. The CDC report, published in the New England Journal of Medicine, focused only on reviewing the evidence linking Zika and fetal anomalies.
Global health officials had already assumed the virus was to blame for the problems being seen in various countries. Since January, many have advised women who were pregnant or hoping to become so to avoid travel to Zika-affected areas or to take steps to avoid Zika infection. That medical advice expanded over time to include women’s partners, especially as it became clear sexual transmission of the virus was more common than had been known.
The research released Wednesday won’t change that advice, officials said. But they are hoping it will help educate the public about the virus and its potential for harm — particularly in the United States.
“We do know that a lot of people aren’t concerned about Zika infection in the United States, and they don’t know a lot about it,” said Sonia Rasmussen, director of CDC’s division of public health information. “It’s my hope that we can be more convincing that Zika does cause these severe birth defects in babies and hope that people will focus on prevention more carefully.”
The research is likely to help scientists developing a vaccine for Zika, she said.
Researchers said there was no “smoking gun” or single definitive piece of evidence that confirmed the virus as causing microcephaly, calcifications within the brain and severe vision and hearing problems. Rather, the findings of recently published studies and a thorough evaluation by CDC researchers using established scientific criteria led them to the conclusion. Frieden likened the process to putting together pieces of a puzzle.
The World Health Organization had said in recent weeks that there was scientific consensus about the virus and microcephaly as well as Guillain-Barré syndrome, a neurological condition that can lead to paralysis. Researchers in Brazil, the hardest-hit country, said this week that Zika also may be associated with a second serious condition similar to multiple sclerosis. In a few cases with adults, swelling of the brain and spinal cord involving the coating around nerve fibers was seen.
CDC officials said they worked independently of the WHO. The U.S. agency is conducting studies on Guillain-Barré syndrome, and officials said they are also likely to make a conclusive link between that condition and Zika. “I think we’re on the same page as the WHO,” Rasmussen said.
There are still many outstanding questions about the risk facing pregnant women infected with Zika. A limited number of studies show the risk ranges from about 1 percent chance of having a baby with microcephaly to almost 30 percent of pregnant women having fetal abnormalities. A study in Brazil identified that upper range, with pregnant women having “grave outcomes,” Rasmussen said.
Scientists also don’t know whether miscarriages and stillbirths are the result of an infection. Nor do they know what stage of pregnancy poses the greatest risk, or whether another infection that occurred at the same time might affect the risk of birth defects, she said.
CDC began its assessment of the evidence last October and included studies that were published on Zika as recently as this past weekend, Rasmussen said. The detailed clinical information shows the most severe forms of microcephaly, also known as fetal brain disruption sequence. In some instances, the babies’ heads are much smaller than what clinicians would normally see, she said.
Among the evidence the report cited to support the causal relationship between Zika and these serious birth defects included:
–Zika infection during critical periods of early pregnancy, usually the first trimester or early second trimester;
–specific, rare patterns of birth defects in fetuses or infants with presumed or confirmed congenital Zika infection;
–biological evidence, including the presence of Zika virus in the brain tissue of fetuses and babies with severe microcephaly who had died.
–rare exposure to the virus and a rare birth defect.
The researchers cited the recent case of a Washington, D.C., woman who tested positive for Zika 10 weeks after she likely contracted an infection during a trip to Guatemala — far beyond what scientists have thought is the case. Damage to the fetus did not show up on early ultrasounds. But after her abortion at 21 weeks, virus was found in the fetal brain and there were significant brain abnormalities.
Brazil normally has an average of 163 cases of microcephaly each year. But since October, officials have confirmed at least 944 cases of microcephaly or other neurological problems, according to the WHO.
After a Zika outbreak in French Polynesia, that island also had an increase in microcephaly cases. It normally has no more than two cases a year, but it saw eight cases during a four-month period in 2014. A recently published study using data from the island estimated the risk for the rare birth condition to be 95 cases of microcephaly for each 10,000 pregnant women infected in the first trimester.
(c) 2016, The Washington Post · Lena H. Sun
{Matzav.com}











